Nail Disorders: How to Tell Fungal Infections Apart from Psoriatic Changes
When your nails start looking weird-yellow, thick, crumbly, or lifting off the nail bed-it’s easy to assume it’s a fungal infection. But what if it’s not? Nail psoriasis can look almost identical, and mistaking one for the other can waste months, cost hundreds of dollars, and make things worse. You’re not alone. Studies show nearly fungal nail infection cases are misdiagnosed as psoriasis, and vice versa. The truth? These two conditions are completely different in cause, progression, and treatment. Knowing the difference isn’t just helpful-it’s essential.
What’s Actually Happening Under Your Nails?
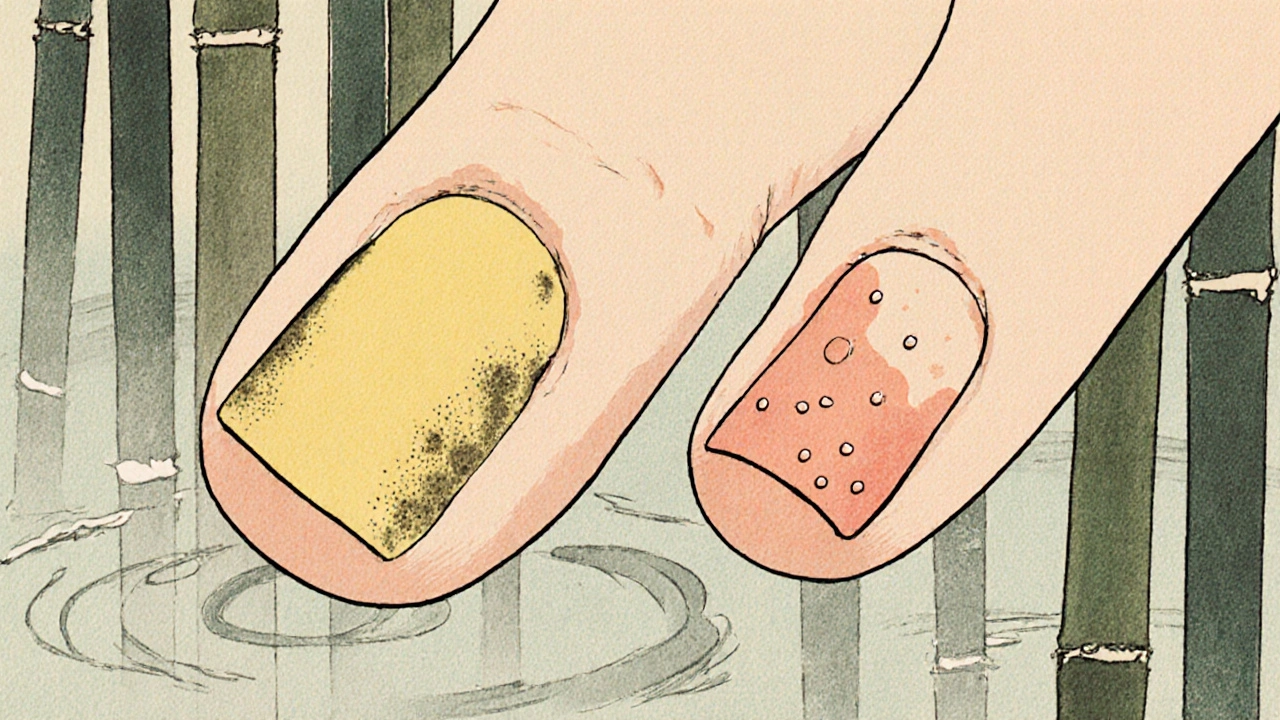
Fungal nail infections, or onychomycosis, are caused by tiny organisms-mostly a type of fungus called Trichophyton rubrum-that invade the nail through small cracks or cuts. They feed on keratin, the protein that makes up your nails. These fungi don’t just sit there. They multiply slowly, pushing deeper over time. You’ll often see a small white or yellow spot near the tip of the nail, then it spreads sideways and downward. The nail gets thicker, discolored (brown or black), and sometimes starts to smell. That foul odor? It’s a red flag. In fact, 40% of fungal infections produce it. Psoriasis doesn’t.
Nail psoriasis, on the other hand, is an autoimmune problem. Your immune system attacks healthy skin cells around the nail, making them grow too fast-every 3 to 4 days instead of every 28 to 30. This messes up the nail’s structure from the inside. You won’t see a spot that grows outward. Instead, you’ll notice multiple nails changing at once, often without any clear starting point. The most telling sign? Pitting. Tiny dents in the nail surface, like someone tapped it with a pin. About 70% of people with nail psoriasis have them. You won’t find those in fungal infections.
Key Differences You Can Spot Yourself
Here’s what to look for when you examine your nails:
- Nail pitting: Small, pinprick-sized depressions. Found in 70% of psoriasis cases. Almost never in fungal infections.
- Salmon patches: Translucent pink or yellowish discoloration under the nail. A classic psoriasis sign.
- Oil-drop lesions: Brownish-yellow spots that look like a drop of oil trapped under the nail. Seen in 15-50% of psoriasis cases.
- Subungual hyperkeratosis: White, chalky buildup under the nail. Happens in almost half of psoriasis cases.
- Foul odor: Strong, unpleasant smell. Present in 40% of fungal infections. Zero in psoriasis.
- Thickening: Both can thicken nails, but fungal infections often cause much more-up to 5mm thick. Psoriasis usually thickens to 2-3mm.
- Pattern of spread: Fungal infections start at the tip or side and creep slowly toward the cuticle. Psoriasis often hits multiple nails suddenly, without a clear origin.
One big mistake people make? Assuming that if it’s on the toenail, it’s fungal. Actually, nail psoriasis affects fingernails 75% of the time. If you have psoriasis on your elbows or scalp, and now your thumbnails are changing, that’s a huge clue.
Why Misdiagnosis Is So Common-and So Costly
Doctors get it wrong about 30-40% of the time. Why? Because the symptoms overlap too much. Yellowing? Both. Thickening? Both. Separation from the nail bed? Both. Even experienced dermatologists sometimes need help.
Here’s what happens when you’re misdiagnosed:
- If you have psoriasis but are treated with antifungal creams or pills, nothing works. Your nails keep getting worse.
- If you have a fungal infection but are given steroid creams for psoriasis, your nail can become even more brittle and start crumbling.
Patients report spending 6 to 12 months trying treatments that don’t work. One Reddit user wrote: “After 8 months of antifungals that did nothing, my nail separated completely and it hurt to touch.” Another said: “My dermatologist said it was psoriasis, gave me steroid cream. My nail turned to dust.”
The economic cost is real. In the U.S. alone, misdiagnosis leads to $850 million in unnecessary spending each year. You’re not just wasting money-you’re wasting time, and your nails are suffering.
How Doctors Actually Diagnose These Conditions
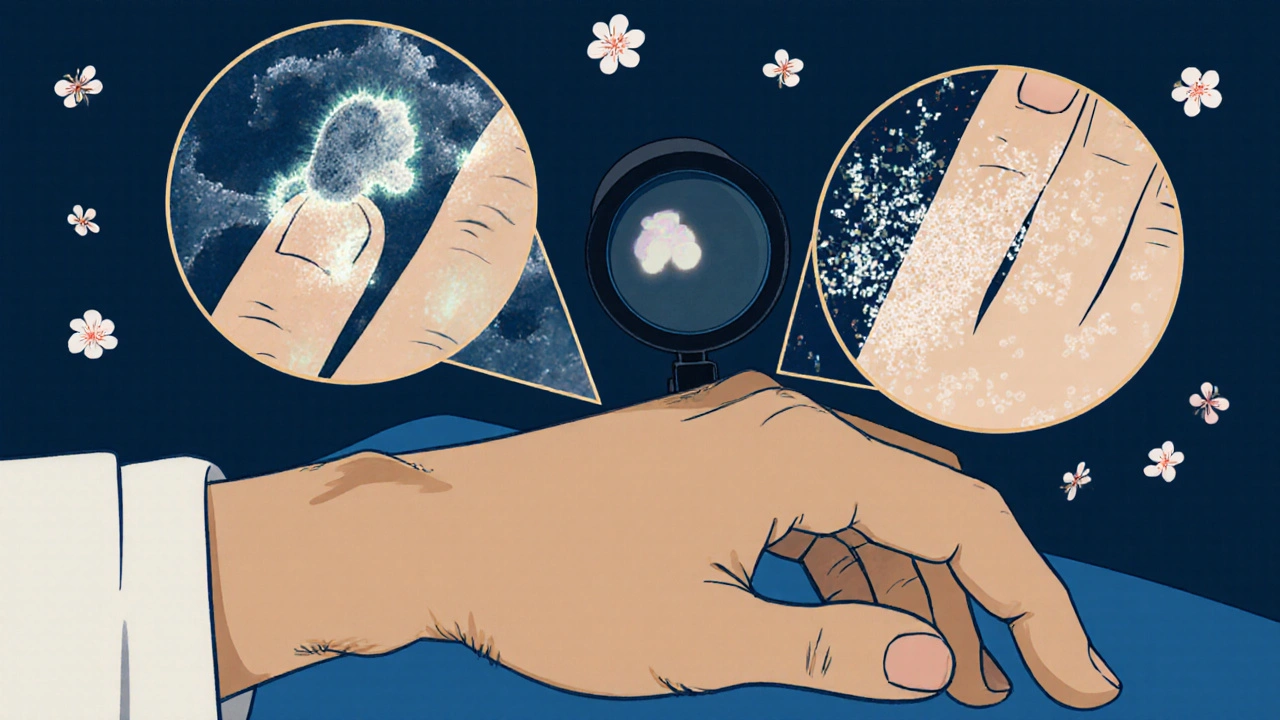
Visual inspection alone isn’t enough. Here’s the step-by-step process professionals use:
- Clinical exam: The doctor looks for pitting, oil spots, salmon patches-signs that scream psoriasis.
- KOH test: A scraping from your nail is mixed with potassium hydroxide and looked at under a microscope. If fungi are there, they glow. This test catches 70-80% of fungal cases.
- Fungal culture: If KOH is negative but suspicion remains, a sample is sent to a lab to grow any fungi. It’s slow-takes 2-6 weeks-but it’s 95% accurate.
- PAS staining: A special dye highlights fungal elements in nail tissue. Used when culture is inconclusive. It’s 90% sensitive.
Some clinics now use reflectance confocal microscopy-a non-invasive imaging tool that lets doctors see the nail structure layer by layer. In a 2023 Mayo Clinic study, it correctly identified the condition in 92% of cases.
For psoriasis, doctors may use the NAPSI score-Nail Psoriasis Severity Index. It breaks the nail into four parts (lunula, matrix, bed, hyponychium) and scores damage in each. It helps track progress over time.
Treatment: What Actually Works
Don’t expect quick fixes. Nail growth is slow-about 0.1mm per day. That means treatment takes months, sometimes over a year.
Fungal Infections
- Oral antifungals: Terbinafine is the gold standard. Taken daily for 12 weeks, it clears the infection in 78% of cases, confirmed by lab tests.
- Topical treatments: Efinaconazole (Jublia) or ciclopirox (Penlac) are applied daily. They work better on mild cases but take 9-12 months for toenails because of slow growth.
- Home care: Keep feet dry. Humidity above 40% helps fungi thrive. Wear breathable shoes. Change socks daily. Disinfect nail clippers and shoes.
Nail Psoriasis
- Corticosteroid injections: Injected directly under the nail, these reduce inflammation. Improvement can show in 8-12 weeks.
- Topical calcipotriene: A vitamin D analog applied daily. Works best when combined with steroid creams.
- Biologics: Drugs like secukinumab (Cosentyx) or ixekizumab (Taltz) target the immune system. In a 2022 survey, 65% of patients saw major improvement after 24 weeks.
- Emollients: Moisturizing the cuticle and nail edges helps prevent separation. Avoid trauma-don’t bite nails, don’t use them as tools.
Important: Steroids can make fungal infections worse. Antifungals won’t help psoriasis. That’s why testing matters.
What You Can Do at Home
Even before you see a doctor, you can help yourself:
- Take monthly photos: Use the same lighting and angle. Compare them over time. Changes in color, thickness, or pitting become obvious.
- Keep nails trimmed short: Reduces pressure and prevents catching on things.
- Don’t share nail tools: Fungi spread easily. Use your own clippers, files, and buffers.
- Watch for triggers: Psoriasis flares after injury, stress, or infection. Fungal infections thrive in damp environments-swimming pools, gyms, showers.
- Track your history: Do you have psoriasis on your skin? Have you had athlete’s foot? These are clues.
The Future: Better Tools on the Horizon
Researchers are making progress. In 2024, Mount Sinai scientists found that the microbes living under your nails differ between psoriasis and fungal infections. Psoriasis nails have more Staphylococcus and less Cutibacterium. Fungal nails show high levels of Trichophyton DNA. Soon, a simple swab test could tell you which condition you have-without a biopsy.
AI is also stepping in. The Global Psoriasis Atlas predicts that by 2027, AI-powered apps analyzing nail photos will reduce misdiagnosis by 22%. Meanwhile, climate change is expanding the habitats of fungi. Experts warn fungal infections could become more common as temperatures rise.
For now, the best tool you have is knowledge. If your nails are changing, don’t guess. Don’t assume it’s fungus because it’s on your toe. Get tested. Know the signs. And remember: what looks like a simple nail problem might be a sign of something deeper.
Can nail psoriasis turn into a fungal infection?
Yes, it can. When psoriasis causes the nail to separate from the nail bed (onycholysis), it creates a gap where fungi can enter. Between 4.6% and 30% of people with nail psoriasis develop a secondary fungal infection. That’s why it’s important to treat psoriasis early and keep the nail area clean and dry.
Will my nails grow back normally after treatment?
It depends. With fungal infections, once the fungus is cleared, the nail usually grows back healthy-but it can take up to a year for toenails. With psoriasis, the nail may return to normal if the underlying condition is controlled. But if the nail matrix (the root) is damaged, permanent changes like pitting or ridges may remain. Early treatment improves outcomes.
Can I treat this at home with vinegar or tea tree oil?
Home remedies like vinegar soaks or tea tree oil might help with mild fungal cases, but they’re not reliable. Studies show they’re far less effective than prescription antifungals. For psoriasis, these won’t help at all. If you’re unsure what you have, don’t delay-see a doctor. Delaying treatment can lead to permanent damage.
Why does my dermatologist keep asking if I have psoriasis on my skin?
Because 95% of people with nail psoriasis have skin psoriasis first-usually 10 to 15 years earlier. If you’ve had scaly patches on your elbows, knees, or scalp, that’s a major clue. Even if your skin looks fine now, psoriasis can be dormant. Nail changes can be the first sign.
Is it safe to get a pedicure if I have a nail disorder?
Be cautious. If you have a fungal infection, public tools can spread it. If you have psoriasis, aggressive filing or cutting can trigger more flares (Koebner phenomenon). If you go, bring your own tools. Avoid soaking nails for long periods. Tell the technician you have a nail condition-they should know how to handle it.
Ravi Kumar Gupta
November 22, 2025 AT 16:18Bro, I had this yellow nail for years and thought it was fungus-turned out it was psoriasis from my scalp eczema. No one ever told me nail changes could be autoimmune. Now I know why antifungals did jack. This post saved me months of wasting cash on pills that made me nauseous.
Rahul Kanakarajan
November 23, 2025 AT 07:00Wow so you're telling me people pay $300 for antifungal creams when they just need to check for pitting? That's ridiculous. I've seen this exact thing in my uncle-he got steroid shots and it cleared in 3 months. Stop guessing and get a KOH test already. This isn't TikTok health advice.
New Yorkers
November 25, 2025 AT 05:51Look, I'm not a doctor but I've read a lot of papers and I think we're missing the bigger picture. The nail isn't just a nail-it's a mirror of systemic imbalance. Fungal infections thrive in toxicity, psoriasis in emotional repression. You can't treat the symptom without addressing the soul. I mean, have you ever considered that your nail is just screaming for you to slow down?
David Cunningham
November 27, 2025 AT 00:42Been there. Had both. Fungal on my big toe, psoriasis on my thumb. The oil-drop thing is dead on. Took me 2 years to figure it out. Just took pics every month like the post said. Best advice ever. Also, don't get pedicures unless you bring your own tools. Saw a guy get a fungal infection from a salon last year. Total nightmare.
james lucas
November 28, 2025 AT 09:25soooo i had this weird thick nail and i thought it was just aging or maybe i stepped on something gross but turns out it was psoriasis?? like i had a little bit of scalp stuff but never connected it. the salmon patch thing blew my mind. also i tried tea tree oil for like 6 months and it did nothing. i just got a steroid injection last month and my nail is already looking better?? like not perfect but way less yellow. also i started using a humidifier because my house is so dry and it helped the cuticles. idk if that matters but it felt good
Jessica Correa
November 29, 2025 AT 23:10My mom had this for years and they kept calling it fungus until she saw a dermatologist who asked if she had psoriasis on her knees. She did. The injections changed everything. Also don't use metal files-plastic ones are gentler. And take photos. Seriously. I didn't believe how much it changed until I compared pics side by side
manish chaturvedi
November 30, 2025 AT 10:25As someone from India where fungal infections are rampant due to humidity and shared footwear, I must emphasize the importance of distinguishing between psoriasis and onychomycosis. Many patients self-medicate with over-the-counter antifungals, worsening the condition. The presence of nail pitting is a critical indicator-often overlooked in primary care. We must educate the public and train clinicians to recognize these signs early. Prevention through hygiene and awareness saves lives and money.
Nikhil Chaurasia
December 2, 2025 AT 07:19I used to think my nail was just dirty until I noticed the tiny dents-like someone poked it with a needle. I was too embarrassed to say anything. Then my cousin mentioned she had psoriasis and I Googled it. Turned out I had it too. I didn’t want to believe it because I didn’t have skin patches. But the nail was the first sign. Thanks for writing this. I feel less alone now.
Holly Schumacher
December 3, 2025 AT 02:59Let me just say this: anyone who recommends vinegar or tea tree oil as a treatment for nail disorders is either dangerously misinformed or actively misleading people. There is zero clinical evidence supporting these remedies for anything beyond superficial fungal spores. Psoriasis? Absolutely useless. Fungal infection? Marginally better than doing nothing, but still 80% less effective than terbinafine. Stop romanticizing home remedies. Get a proper diagnosis. Your nails deserve better than Pinterest hacks.
Michael Fitzpatrick
December 4, 2025 AT 17:31I just want to say how much I appreciate this post. I’ve been dealing with nail changes for over a year and felt so lost-everyone just told me to ‘try this cream’ or ‘soak in vinegar.’ But this actually gave me a roadmap. I got the KOH test last week and turns out I had a mild fungal infection. Started terbinafine and already feel hopeful. Also, the part about taking monthly photos? Genius. I started doing that and I can actually see the new nail growing in. It’s slow but it’s happening. Thank you for not just listing symptoms but giving real hope.
luke young
December 5, 2025 AT 09:54Just want to add-don’t ignore the Koebner phenomenon. I had psoriasis on my elbow, got a tiny cut from a nail clipper, and boom-new psoriasis spot on my finger. Same thing with nails. Be gentle. Don’t pick. Don’t file aggressively. Even stress can flare it. I started meditating and my nails improved. It’s not just about medicine. It’s about how you treat your whole body.